When I start working with a new diabetes or weight management client, I introduce the idea of the 4-hour gut rest. Many times, I get the response of “But aren’t I supposed to have snacks?”
In a word, no. Why is that? What difference does it make whether I eat in the next 30 minutes or 3 hours? Let’s start with unpeeling digestion.
How long does it take food to digest?
Below is the amount of time it takes to go through each part of the Alimentary Canal. Alimentary Canal is the term for your entire digestive tract – from your mouth to what you may currently be sitting on.
- Mouth – 10 seconds, and I am being generous, for a bite of food to finish being chewed.
- Esophagus – 2-3 seconds
- Stomach – Usually between 50 minutes to 2 hours depending on what and how much you ate
- Small Intestines – Approximately 7 hours
- Large Intestines – Approximately 36 hours. Yep, your food hangs out the longest amount of time in your colon. I will write about what is going on down there and the gut biome in future weeks.
How does glucose effect the bloodstream?
Here are the steps that your body takes after you eat food in a healthy body:
- You eat breakfast.
- Your enzymes begin to digest the food, starting with enzymes in your mouth, and releasing glucose into the blood stream.
- This enzymatic action signals the pancreas to release insulin.
- The insulin enters the blood stream and goes to your cells and works like a key to open the door of the cell.
- The glucose goes into the cell and gives the cell the energy to do its function, whether that be to run your heart, move nerve stimuli down your arm or have your eye blink.
- Life is good.
If that is all working correctly, you will have a blood glucose spike for about 2 hours. But you may have noticed that according to the digestion timeline, your stomach has barely emptied. Also, when you have a blood glucose disorder, as in diabetes, your system is compromised. It will probably take longer for your spike to come down to what we call pre-prandial, or “before you ate” level.
You may have had a Glucose Tolerance Test[i] when you were first diagnosed with diabetes. The reason for that was to find out what happens to your blood sugars when you get a large dose of glucose. How high do you spike? (Shows how much glucose and fiber was in your food.) How long does it take to bring down the spike? (Shows how well your pancreas is working.)
If you are thinking that you may need this information and you haven’t had a glucose tolerance test, this is what happens during a the test. There will be 4 blood draws.
- Before you drink a very sugary drink.
- Anywhere from 30 to 60 minutes after your drink the sugary drink.
- Again, after another hour.
- Again, after another 30 to 60 minutes.
A healthy glucose spike is within 40 points. So, if you are a healthy person, you will start out somewhere under 99 mg/dL. Then spike around 140 mg/dL after the first hour and back down to under 99 mg/dL after the next hour.
But what happens if your blood sugar is still up after 2 hours? This relates back to the original question about 4-hour gut rests.
If your glucose level is still high and you eat more food, it goes even higher. So, instead of starting out under 99 mg/dL, you now are starting at 120 mg/dL. Even if you have a spike in the healthy range of 40 mg/dL, your blood glucose level is now 160 mg/dL. Eat again in another 2 hours and you will be starting again higher than 99 mg/dL and spiking higher.
Also, realize that your stomach may not be totally empty after 2 hours. It is dumping its’ contents into the small intestines. The enzymes to digest your food are returning to pre-prandial levels. But, you are putting in more food. This signals the stomach enzymes to rev back up again. This is stressing the body.
Here’s another action going on. Your body sends blood to the stomach to help digest food. You are supposed to be done with digesting before putting anything else in, but now, you are adding a snack. Even if it is a healthy snack, your gut has not had any time to get back to a rested state.
According to Waaler and Toska, “ . . . blood flow to the [intestinal] tract increases gradually and markedly after a meal, and more so after a big meal than after a small one. The increase in blood flow reaches its maximum after 20-40 minutes and lasts for 1.5-2 hours. In the postprandial [after meal] period there is a parallel and similar increase in cardiac output; the meal thus imposes an increased workload on the heart.” [ii]
This means that in addition to the lack of rest for the stomach and small intestines, the heart is also stressed.
Let’s recap –
- You want a cookie at 2:30pm after your lunch was done at 1:30.
- Your stomach hasn’t really emptied and the enzymes to break down food are back in action.
- Your blood glucose hasn’t returned to the premeal level, and you are adding more glucose to the system.
- Your blood is still in the stomach area putting stress on the heart and you are going to continue the stress.
Oops I forgot something else that was going on – your pancreas was making insulin.
What does insulin do after a meal?
You ate a really healthy lunch of a big salad with chickpeas and my Creamy Cashew Dressing. You are being great today.
Your pancreas pumped out insulin to help the glucose get into your cells. Insulin is a response to there being a certain amount of glucose in the bloodstream. If there is a high dose of glucose, higher than the insulin can get into the cells, your body begins to turn the glucose into fat.
Back to the cookie thing.
When you have a high fiber meal, like this salad, the glucose is slowed to release. But now, before the glucose in the blood stream is back to a pre-prandial or pre-meal level, you are adding more glucose. The threshold of insulin turning glucose into fat is much sooner than before you ate the salad. Additionally, since there isn’t much fiber in the cookie, the glucose will be released easily.
Doesn’t eating frequently help you lose weight?
When researching weight loss, researchers measure Body Mass Index (BMI). Body Mass Index is your height versus your weight, basically. It is a good number to start and measure where you are in the range, key word here RANGE, of a healthy weight. Very muscular people, or body builders can throw it off because even though they have a very low-fat body mass and are healthy, the weight of their muscles doesn’t compute with the formula. That being said, most of us are not body builders or super athletes and can use the BMI to calculate whether or not we are within a healthy weight range.
Kahleova and colleagues found that eating one or two meals daily was associated with a relatively lower BMI compared with three meals daily. Interestingly, they found that if the number of meals and snacks were more than three daily there was an increase in BMI. So, no, the research longer than a couple of weeks shows that more than 3 meals daily leads to a higher BMI. Below is a graphic from their paper, used with permission, surmising their findings.
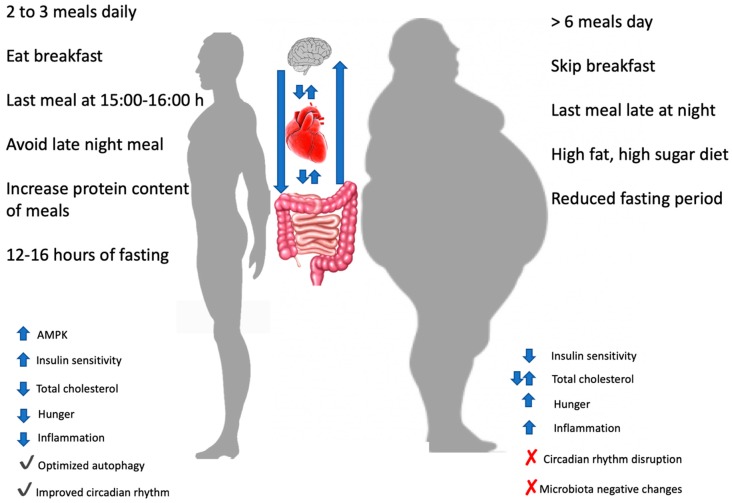
But here is the interesting thing.
It wasn’t just the snacks, the change in BMI was related to the length of the overnight fast.
What does overnight fast mean?
I also recommend that you have at least 12 hours between the last meal of Day 1 and the first meal of Day 2. This gives the body the time needed to repair itself while you are winding down and sleeping. What Kahleova, et al,[ii] saw was that the longer the overnight fast, the lower the BMI.
As you may know from your life with diabetes or knowing someone with diabetes, they need to have steady mealtimes.[iii] That is not just a good idea but also supports the circadian rhythms of many cycles in your body.
What is a circadian rhythm?
Circadian rhythms are physical, mental, and behavioral changes that follow a 24-hour cycle. These natural processes respond primarily to light and dark and affect most living things, including humans.[iv] And just like the sun going down tells your body to start making melatonin to help your sleep, having steady mealtimes, that end by 7pm, helps your gut do its job.
Researchers found that disrupting the timing, for example, jetlag, can disturb normal peripheral and central clocks in the body. Desynchronizing these internal clocks increased risks of metabolic and cardiovascular diseases. A chronic clock misalignment has been demonstrated to promote glucose intolerance and obesity.
Interestingly, you have more than just one clock syncing. You have clocks regulating your sleep cycle, metabolism cycle, digestive cycle, hormonal cycle and a newly emerging one: The gut microbiota.
This gives the body around 13 hours to rest and repair itself without having to stress with digestion.
What is the Gut Microbiota[v]
The gut microbiota is a vast and complex collection of microorganisms throughout the alimentary canal that profoundly affects human health. This is where the idea of the “Second Brain” or “gut-brain axis” comes from. The brain in your head uses the same nerve pathways as the nerves in the gut microbiota.
Paoli, et al. wrote in a recent review that interrupting the syncing of internal clocks modifies the microbiota and may increase risks of metabolic and cardiovascular diseases; and may promote glucose intolerance and obesity.[vi]
What does gut rests look like in real life?
Using a 4 hour gut rest is not difficult. In fact, when you put it into action, your day becomes simpler. The best thing I realized was that I immediately knew when I needed to take food on the go. It clarified when I needed to take a break and put together a meal. It also helped me know what I needed to prep for the week or the night before. Using gut rests in real life it looks like this:
- You get up at 7:00am and eat at 8:00am
- Your next meal isn’t until at least 12:00pm. You can definitely have all the water and herbal tea you want with no added sweetener. It is fine if your second meal is later. Just not before.
- Your evening meal isn’t until at least 4:00pm and is completed by 7:00pm.
This gives the body around 13 hours to rest and repair itself without having to stress with digestion.
Having rests between meals may be a good idea to your brain, but to the rest of your body on circadian rhythms and needing to repair itself, it is really the law.
[i] https://www.mountsinai.org/health-library/tests/glucose-tolerance-test-non-pregnant
[i] Waaler, B. A., & Toska, K. (1999). Fordøyelseskanalens store og vekslende behov for blodtilførsel [Digestive system’s large and changing needs of blood supply]. Tidsskrift for den Norske laegeforening : tidsskrift for praktisk medicin, ny raekke, 119(5), 664–666.
[ii] Kahleova, H., Lloren, J. I., Mashchak, A., Hill, M., & Fraser, G. E. (2017). Meal frequency and timing are associated with changes in body mass index in Adventist Health Study 2. The Journal of nutrition, 147(9), 1722-1728.
[iii] Paoli, A., Tinsley, G., Bianco, A., & Moro, T. (2019). The Influence of Meal Frequency and Timing on Health in Humans: The Role of Fasting. Nutrients, 11(4), 719. https://doi.org/10.3390/nu11040719
[iv] https://nigms.nih.gov/education/fact-sheets/Pages/circadian-rhythms.aspx#:~:text=%E2%80%8B%E2%80%8BWhat%20are%20circadian,the%20study%20of%20circadian%20rhythms.
[v] https://www.medicalnewstoday.com/articles/307998#the-gut-microbiota
[vi]Ibid 4